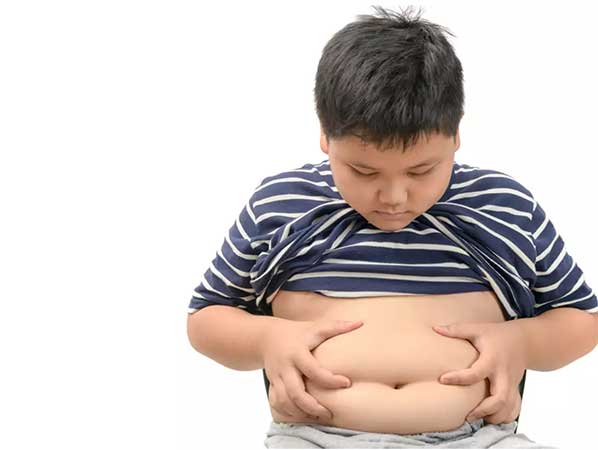
Changes in blood fats and other markers of heart health and diabetes detectable from age of six in children with overweight, Danish study finds
- Early childhood – as young as 2.5 years old – provides critical window to detect overweight
- Early detection could provide crucial opportunity to improve a child’s health for years to come
A new study being presented at this year’s European Congress on Obesity (ECO) in Maastricht, the Netherlands, and published simultaneously in Obesity Research & Clinical Practise, has revealed that changes in blood fats and other markers of heart health and diabetes are detectable from the age of six in children who have overweight.
The study of almost 1,000 Danish children also established that routine dental check-ups provide a good opportunity to measure BMI.
“The prevalence of childhood obesity is high and the short-term and long-term complications of childhood obesity are numerous,” says the study’s first author, Dr Christine Frithioff-Bøjsøe, of the Children’s Obesity Clinic, European Centre for Obesity Management, Copenhagen University Hospital Holbaek, Holbaek, Denmark.
“Overweight in early childhood often tracks into adolescence and adulthood and is associated with a higher risk of heart disease, liver disease, type 2 diabetes and other metabolic conditions in later life. As a result, the early identification and treatment of overweight provides a crucial opportunity to improve a child’s health for years to come.”
The study which was led by Dr Frithioff-Bøjsøe, Prof Jens-Christian Holm and colleagues at the Children’s Obesity Clinic, set out to discover if it is practical to use existing contacts in primary healthcare sector to detect overweight from an early age.
Dental assistants and public health nurses were trained in measuring weight and height and carried out BMI assessments during routine appointments in dental clinics (children in Denmark are entitled to regular dental appointments from as early as the age of one) and in health visits in schools.
The dental assistants recruited 335 pre-school children (age 2.5 and 5 years old) into the study. A further 657 school-age children (6-8 years old) were recruited by public health nurses, taking the total number of participants to 992 (494 boys).
All the children had their BMI assessed at the start of the study. A sub-group of 392 children had their blood pressure measured and gave a blood sample, which was tested for a range of cardiometabolic risk markers.
The BMI assessments and other tests were repeated approximately a year later.
At the start of the study, the proportion of children with overweight was 13.7% in both groups (pre-school children and schoolchildren).
Differences in cardiometabolic risk markers between children with and without overweight were minor in the pre-schoolers.
In the schoolchildren, however, there were clear differences in the blood test results between those with overweight and those in the normal weight range.
Schoolchildren with overweight had significantly higher levels fasting glucose, insulin, triglycerides and alanine aminotransferase, which can indicate a higher risk of type 2 diabetes, cardiovascular disease and liver disease.
Levels of overweight hadn’t changed in the pre-school children when they were measured again around a year later but had risen to 17% in the schoolchildren.
The study’s authors say that their research shows that it is practical to use existing health services, including dental clinics, to evaluate the degree of overweight in a general paediatric population.
Dr Frithioff-Bøjsøe adds: “We also overcame barriers identified in other studies which include concerns about a lack of adequate training, offending patients and caregivers and stigmatisation of the child.”
The researchers say that even though the risk marker levels measured in the study were still in normal range, the increases are still a concern, particularly at such a young age.
Dr Frithioff-Bøjsøe explains: “By the age of 11, 15-20% will exhibit overweight and a large group will subsequently exhibit high blood cholesterol levels, fatty liver disease or prediabetes, as well as a severely affected quality of life. So, detecting these changes early would be a major advance in preventing the development of disease.”
The authors conclude: “We found rises in risk markers for heart and liver disease and diabetes in schoolchildren with overweight. These changes were not detectable just a few years earlier in pre-schoolers with overweight and suggests that pre-school – as early as 2.5 years of age – could provide a critical window to detect and manage overweight.
“This would, in turn, allow weight loss interventions to start early, and reduce the risk of a child with overweight becoming an adult, or even an adolescent, with overweight and other conditions such as type 2 diabetes.”
https://www.journals.elsevier.com/obesity-research-and-clinical-practice