On primary care leadership
Authors: John Spicer, Acting Dean of GP and Community Based Education London
Francesco Carelli, Professor of Family Medicine Milan, Rome
It is good to lead.
It is axiomatic that it is good to lead.
For differing reasons around Europe leadership is celebrated and actively promoted in primary care circles. It is apposite to consider why this might be so, what it might mean and whether it is of value. Initially the challenges facing European health care in general, and primary care in particular could be said to call for leadership – there is a perception of crisis in many countries health care systems for example . Crisis in funding and organisations to name but two, and good leadership among other factors can help address it by facilitating new ideas and practical responses.
Let us start with an example.
A group of interested health care professionals is called together by one of their members to consider provision of musculo-skeletal services in a district. Physiotherapy waiting times in primary care are around 26 weeks for simple problems and there is much negative comment from referrers and patients. Cost constraints are required.
A meeting is chaired by the chief local physiotherapist who invites contributions from GPs, OTs, rheumatologists et al.
After some discussion, a paper on referral guidelines is tabled and the GPs are asked to consider implementing them at the start of the next financial year, a date which is 2 months ahead
This sort of interaction is everyday, in any health care system. The UK National Health Service is promoting a relatively new approach to developing leadership skills in medical, and by extension, health care professionals. This Medical Leadership Competency Framework outlines all the skills held to be necessary in our clinician-leaders.
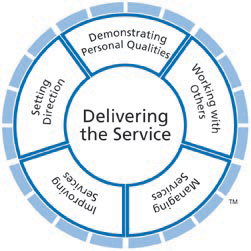 Clearly thechair of the meeting above finds herself, perhaps by design, perhaps by accident , in a leadership role, and if she is to push, lead or drive the process on she is going to need something of the 5 qualities in the outer circle above. Under this framework each of the five domains are further divided into more component parts and the reader is directed to sources such as that referenced for more detail on these aspects.
Clearly thechair of the meeting above finds herself, perhaps by design, perhaps by accident , in a leadership role, and if she is to push, lead or drive the process on she is going to need something of the 5 qualities in the outer circle above. Under this framework each of the five domains are further divided into more component parts and the reader is directed to sources such as that referenced for more detail on these aspects.
Let’s think about that meeting in a little more detail: clearly the chair will be exercising leadership if only in keeping the meeting on task and getting to some sort of output, a plan for the future perhaps. She might do that in any of the styles described by Heron as below:
Hierarchical leaders are just that. They lead from the front, in the manner of ancient kings before their armies, issue instructions and expect to be obeyed. Sometimes they are right.
Co-operative leaders work with their groups to evolve, in a democratic manner, the best way to do things. Autonomous leaders leave it to their charges to work things out, and may be the voice of the group who says what it is collectively held to be correct.
She may have a vision of how she wants the output to be and direct the meeting accordingly [hierarchical style] or she may leave the members to find their own way [autonomous style] . She may steer a course in between, hearing the members voices and shaping their contributions [co-operative style] It is likely that a good leader can use each of these styles where the need arises.
So the meeting is a microcosm of the various professionals who all have a role in determining good practice and good health provision – they are liable to be disparate, eclectic and multi skilled. Their perspectives will be different. Arguably they are not all primary care practitioners, but they should all have good care and good outcomes as shared aims.
The view point from primary care includes several key features: it is the point of first contact for the patient, it is the domain of the expert generalist and it is the epicentre of long term care and continuity. Our contention is that these descriptors of work do not substantially affect the implementation of good leadership from other domains of care. Theoretical aspects are naturally conjoined with practical.
To return to the case: it is notable that the chair, and a species of leader in that role, is by profession a physiotherapist. It is a historical accident that doctors have always tended to have more direct power in the interprofessional context, and the reasons underlying that state of affairs probably go beyond this brief review. However the leadership of the multidisciplinary primary care team could be usefully compared with the secondary care team, though both are subject to the same historical accident. The nature of primary care is distributed geographically and does not lie within the convenient four walls of a hospital or equivalent institution – so there is less chance, or more effort required to bring a team together. The physiotherapist chair will be addressing members who may not even regard themselves as a team, but more a virtual gathering; and this might bring a different challenge to the task of leading them to agreement in this service reconfiguration. Through most of Europe a transformation is pending in care delivery, where even more work is to be transferred from secondary to primary care, or at least integrated more closely together to enhance the patient journey. Referral management, the implication of the case example, is a reality both for cost containment and , perhaps, better patient care.
What we should ask en passant does primary care in this context: hitherto we have used the term freely and without definition. The truth is that the term applies to many different varieties of care around the world. Universally, primary care is about first access, where a patient sees a primary care clinician about an issue as the first point of call. So there is an undifferentiated pattern about the nature of the presenting problem. Generally the primary care clinician sees his or her patient in their own milieu, and takes a biographical as well as a biotechnical approach to care. Given these arguably universal characteristics [and it is self-evident that other characteristics will be applied in different countries around the world] how may leadership structure and function differ ?
Taking the larger view, but consistent with the view of the case above as a microcosm of everyday primary care, let us consider some wider issues. We started this article with a statement about crisis – of funding, of organisation and of professional role.
A new system cannot go forward without co-operation and a democratic sharing of responsibilities. Historically primary care teams have been led by general practitioners : this has meant leadership of local teams as in our example, but it may also mean professional leadership as family medicine where family medicine takes systems leadership. There is plenty of evidence that population health outcomes are best where there is strong primary care, and perhaps general practitioners do need to step forward as leaders of primary care teams, at least for the moment, to drive forward positive change. Despite its general complexity and perverse incentive that may be one side effect of the UK NHS and Social Care Act 2013. Congruent leadership, as it has been called, seeks to bring together the clinical responsibilities and larger systemic or societal responsibilities of clinician – leaders, a position with we recommend
References
Austerity: a failed experiment on the people of Europe McKee, M; Karanikolos, M; Belcher, P; Stuckler, D, Journal of the Royal College of Physicians, [2012], vol. 12, no. 4, pp. 346-350(5)
Leadership theories and the development of nurses in primary health care Taylor R [2009] Primary Health Care [19] 9 40-45
In command of care: Toward the theory of congruent leadership Stanley D Journal of Research in Nursing March 2006 vol. 11 no. 2 132-144



