Single men “less likely” to participate in bowel screening
Single men are significantly less likely to participate in bowel screening tests compared to those who live with a partner, according to a new University of Stirling study.
 The findings are among the first to emerge from a pioneering study, Healthy Ageing in Scotland (HAGIS), which has collated comprehensive data on the economic, health and social circumstances of over 1,000 Scots aged 50+ years.
The findings are among the first to emerge from a pioneering study, Healthy Ageing in Scotland (HAGIS), which has collated comprehensive data on the economic, health and social circumstances of over 1,000 Scots aged 50+ years.
This comprehensive study of ageing is the first of its kind in Scotland and will join the Gateway to Global Aging platform, which influences and informs public policy worldwide by supporting international ageing research.
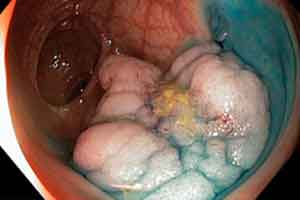
As part of the study, participants were asked whether they had ever taken part in the Scottish Bowel Screening Programme, which is credited with saving 150 lives a year.
Since 2009, Scots aged 50 and over have the option of taking the free test, which involves sending three samples of faeces to a local NHS laboratory, every two years. Screening is proactively offered to people aged between 50 and 74, while those 75 and over can participate on request.
The study found 74.7 per cent of those surveyed had ever taken part in the screening programme but it varied significantly depending on living arrangements and gender. In the case of men living with a partner, 79.5 per cent had taken the test, however, that figure fell to 57.6 per cent for those who lived alone.
In women, 77.8 per cent of those living with a partner had taken the test compared to 73.3 per cent of those living alone.
Principal Investigator David Bell, Professor of Economics at Stirling Management School, said: “Our research indicates that men are significantly less likely to accept the offer of a free bowel screening test if they are living alone, compared to those who have a partner.
“We believe this could be attributed to the support that partners offer each other in terms of encouraging each other to take part in the test. Those living with a partner also have someone to discuss the screening process with, helping to allay concerns and fears.”
The research found that the participation rate of the youngest age group
(50-54) was 58.7 per cent and that the rate increased with age. Of those aged 55 to 59, 67.5 per cent had taken a test, followed by 60-64 (77%),
65-69 (81.9%), 70-74 (77.8%) and 75-79 (79.5%).
Uptake was also lower in deprived communities, the research found. However, there did not seem to be a disparity in the participation rate between those living in urban and rural areas. The team said this “was not surprising”
given the screening was conducted by post.
Professor Bell added: “We believe our findings could help to inform and shape health policy to ensure future campaigns can be targeted at those who are less likely to participate, such as males living alone in deprived areas.
“Ultimately, if the participation rate can be increased, more lives will be saved.”
Source: University of Stirling